In recent days, the world has watched with curiosity and growing alarm as scientists in the U.K. have described a newly identified variant of the coronavirus that appears to be more contagious than, and genetically distinct from, more established variants. Initial studies of the new variant prompted Prime Minister Boris Johnson to tighten restrictions over Christmas, and spurred officials in the Netherlands, Germany and other European countries to ban travel from the U.K.
The new variant is now the focus of intense debate and analysis. Here’s some of what scientists have learned so far.
Is the U.K. variant some kind of new supervirus?
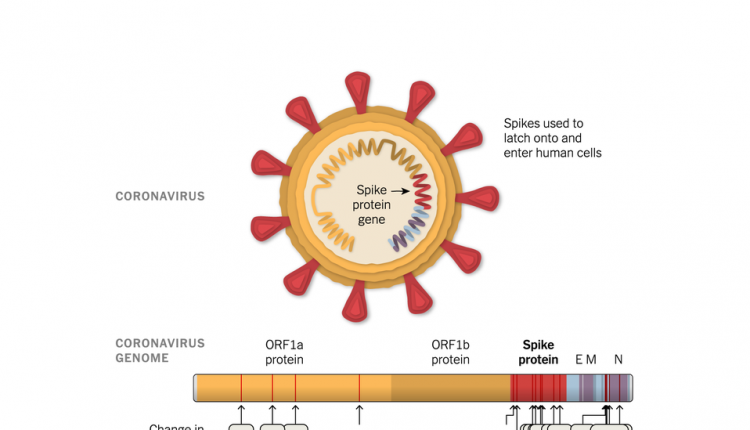
No. It’s just one variation among many that have arisen as the coronavirus SARS-CoV-2 has spread around the world. Mutations arise as the virus replicates, and this variant — known as B.1.1.7 — has acquired its own distinctive set of them.
What is unusual about it?
The variant came to the attention of researchers in December, when it began to turn up more frequently in samples from parts of southern England. It turned out to have been collected from patients as early as September.
When researchers took a close look at its genome, they were struck by the relatively large number of mutations — 23, all told — that it had acquired. Most mutations that arise in the coronavirus are either harmful to the virus or have no effect one way or another. But a number of the mutations in B.1.1.7 looked as if they could potentially affect how the virus spread.
Is it more contagious than other viruses?
It appears so. In preliminary work, researchers in the U.K. have found that the virus is spreading quickly in parts of southern England, displacing a crowded field of other variants that have been circulating for months.
However, a virus lineage becoming more common is not proof that it spreads faster than others. It could grow more widespread simply through luck. For instance, a variant might start out in the middle of a crowded city, where transmission is easy, allowing it to make more copies of itself.
Still, the epidemiological evidence gathered so far from England does seem to suggest that this variant is very good at spreading. In places where it has become more common, the overall number of coronavirus cases is spiking. Neil Ferguson, an epidemiologist at Imperial College London, estimates that the variant has an increased transmission rate of 50 to 70 percent compared to other variants in the United Kingdom.
Some scientists have raised the possibility that the increase in transmission is at least partly the result of how it infects children. Normally, children are less likely than teenagers or adults to get infected or pass on the virus. But the new strain may make children “as equally susceptible as adults,” said Wendy Barclay, government adviser and virologist at Imperial College London.
To confirm that the variant truly is more contagious, researchers are now running laboratory experiments on it, observing up close how it infects cells.
Researchers have already used such experiments to investigate a mutant that arose earlier in the pandemic, called 614G. That variant proved to be more transmissible than its predecessors, studies in cell culture and animals found.
But disciplined containment measures worked just as well against 614G as other variants. The same is likely true for B.1.1.7. “According to what we already know, it does not alter the effectiveness of social distancing, face masks, hand washing, hand sanitizers and ventilation,” Dr. Muge Cevik, an infectious disease specialist at the University of St. Andrews School of Medicine, said on Twitter.
Covid-19 Vaccines ›
Answers to Your Vaccine Questions
With distribution of a coronavirus vaccine beginning in the U.S., here are answers to some questions you may be wondering about:
-
- If I live in the U.S., when can I get the vaccine? While the exact order of vaccine recipients may vary by state, most will likely put medical workers and residents of long-term care facilities first. If you want to understand how this decision is getting made, this article will help.
- When can I return to normal life after being vaccinated? Life will return to normal only when society as a whole gains enough protection against the coronavirus. Once countries authorize a vaccine, they’ll only be able to vaccinate a few percent of their citizens at most in the first couple months. The unvaccinated majority will still remain vulnerable to getting infected. A growing number of coronavirus vaccines are showing robust protection against becoming sick. But it’s also possible for people to spread the virus without even knowing they’re infected because they experience only mild symptoms or none at all. Scientists don’t yet know if the vaccines also block the transmission of the coronavirus. So for the time being, even vaccinated people will need to wear masks, avoid indoor crowds, and so on. Once enough people get vaccinated, it will become very difficult for the coronavirus to find vulnerable people to infect. Depending on how quickly we as a society achieve that goal, life might start approaching something like normal by the fall 2021.
- If I’ve been vaccinated, do I still need to wear a mask? Yes, but not forever. Here’s why. The coronavirus vaccines are injected deep into the muscles and stimulate the immune system to produce antibodies. This appears to be enough protection to keep the vaccinated person from getting ill. But what’s not clear is whether it’s possible for the virus to bloom in the nose — and be sneezed or breathed out to infect others — even as antibodies elsewhere in the body have mobilized to prevent the vaccinated person from getting sick. The vaccine clinical trials were designed to determine whether vaccinated people are protected from illness — not to find out whether they could still spread the coronavirus. Based on studies of flu vaccine and even patients infected with Covid-19, researchers have reason to be hopeful that vaccinated people won’t spread the virus, but more research is needed. In the meantime, everyone — even vaccinated people — will need to think of themselves as possible silent spreaders and keep wearing a mask. Read more here.
- Will it hurt? What are the side effects? The Pfizer and BioNTech vaccine is delivered as a shot in the arm, like other typical vaccines. The injection into your arm won’t feel different than any other vaccine, but the rate of short-lived side effects does appear higher than a flu shot. Tens of thousands of people have already received the vaccines, and none of them have reported any serious health problems. The side effects, which can resemble the symptoms of Covid-19, last about a day and appear more likely after the second dose. Early reports from vaccine trials suggest some people might need to take a day off from work because they feel lousy after receiving the second dose. In the Pfizer study, about half developed fatigue. Other side effects occurred in at least 25 to 33 percent of patients, sometimes more, including headaches, chills and muscle pain. While these experiences aren’t pleasant, they are a good sign that your own immune system is mounting a potent response to the vaccine that will provide long-lasting immunity.
- Will mRNA vaccines change my genes? No. The vaccines from Moderna and Pfizer use a genetic molecule to prime the immune system. That molecule, known as mRNA, is eventually destroyed by the body. The mRNA is packaged in an oily bubble that can fuse to a cell, allowing the molecule to slip in. The cell uses the mRNA to make proteins from the coronavirus, which can stimulate the immune system. At any moment, each of our cells may contain hundreds of thousands of mRNA molecules, which they produce in order to make proteins of their own. Once those proteins are made, our cells then shred the mRNA with special enzymes. The mRNA molecules our cells make can only survive a matter of minutes. The mRNA in vaccines is engineered to withstand the cell’s enzymes a bit longer, so that the cells can make extra virus proteins and prompt a stronger immune response. But the mRNA can only last for a few days at most before they are destroyed.
Does it cause more severe disease?
There is no strong evidence that it does, at least not yet. But there is reason to take the possibility seriously. In South Africa, another lineage of the coronavirus has gained one particular mutation that is also found in B.1.1.7. This variant is spreading quickly through coastal areas of South Africa. And in preliminary studies, doctors there have found that people infected with this variant carry a heightened viral load — a higher concentration of the virus in their upper respiratory tract. In many viral diseases, this is associated with more severe symptoms.
Where did this unusual variant come from?
That is now a question of intense debate. One possibility is that the variant gained its array of new mutations inside a special set of hosts.
In a typical infection, people pick up the coronavirus and become infectious for a few days before showing symptoms. The virus then becomes less abundant in the body as the immune system marshals a defense. Unless patients suffer a serious case of Covid-19, they typically clear the virus completely in a few weeks at most.
But sometimes the virus infects people with weak immune systems. In their bodies, the virus can thrive for months. Case studies on these immunocompromised people have shown that the virus can accumulate a large number of mutations as it replicates in their bodies for a long period of time.
Over time, researchers have found, natural selection can favor mutant viruses that can evade the immune system. Researchers have also suggested that the evolution of the variant might have been additionally driven by medicine given to such patients. Some mutants might be able to withstand drugs such as monoclonal antibodies.
Other scientists have suggested that the virus could have gained new mutations by spreading through an animal population, like minks, before re-entering the human population. Such “animal reservoirs” have become a focus of intense interest as more animal infections have been detected.
Is the variant already circulating in the U.S.?
Not yet, as far as anyone knows. But that does not mean it hasn’t already reached the United States. British scientists have established a much stronger system to monitor coronaviruses for new mutations. It’s conceivable that someone traveling from the United Kingdom has brought it with them. Now that the world knows to look for the variant, it may turn up in more countries.
Will the variant render the new vaccines ineffective?
No. Most experts doubt that it will have any great impact on vaccines, although it’s not yet possible to rule out any effect.
The U.S. Food and Drug Administration has authorized two vaccines, one from Moderna and the other from Pfizer and BioNTech. Both vaccines create immunity to the coronavirus by teaching our immune systems to make antibodies to a protein that sits on the surface of the virus, called spike. The spike protein latches onto cells and opens a passageway inside. Antibodies produced in response to the vaccines stick to the tip of the spike. The result: The viruses can’t get inside.
It is conceivable that a mutation to a coronavirus could change the shape of its spike proteins, making it harder for the antibodies to gain a tight grip on them. And B.1.1.7’s mutations include eight in the spike gene. But our immune systems can produce a range of antibodies against a single viral protein, making it less likely that viruses can easily escape their attack. Right now, experts don’t think that the variant will be able to evade vaccines. To confirm that, researchers at the Walter Reed Army Institute of Research are analyzing the changes to the structure of its spike protein.
Dr. Moncef Slaoui, the head scientific adviser to Operation Warp Speed, the federal effort to deliver a vaccine to the American public, said that the new variant reported in Britain was unlikely to affect the efficacy of a vaccine.
At some point — “some day, somewhere” — a variant of the virus may make the current vaccine ineffective, he said, but the chance of that happening with this vaccine is very low. Nevertheless, he said, “we have to remain absolutely vigilant.”
But Kristian Andersen, a virologist at Scripps Research Institute, thinks it is too early to dismiss the risk to vaccines. If the U.K. variant evolved to evade the immune system in immunocompromised patients, those adaptations might help it avoid vaccines. The vaccines would not become useless, but they would become less effective. Fortunately, experiments are underway to test that possibility.
“We don’t know, but we’ll know soon,” Dr. Andersen said.
Benjamin Mueller and Katie Thomas contributed reporting to this article
[Like the Science Times page on Facebook. | Sign up for the Science Times newsletter.]

Comments are closed.