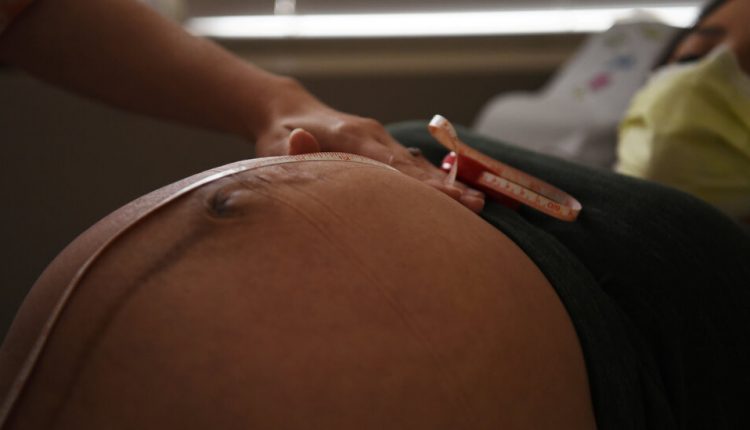
With the emergency approval of the Pfizer BioNTech vaccine on Friday evening, the Food and Drug Administration took an unexpected step, leaving open the possibility that pregnant and breastfeeding women might opt for immunization against the coronavirus.
The agency approved the vaccine for people 16 years and older and asked Pfizer to submit regular reports on the vaccine’s safety, including its use in pregnant women.
There was no guarantee the agency would take this route. The vaccine has not been tested in women who are pregnant or breastfeeding. UK regulators recommended that these women receive the shots, although they recognized that the evidence so far “does not raise concerns about safety in pregnancy”.
The Centers for Disease Control and Prevention has not yet approved the vaccine for pregnant women, but an advisory committee from the agency is expected to meet this weekend to make further recommendations.
Some experts said the virus itself posed a higher risk to pregnant women than the new vaccine, noting that vaccines have been given to pregnant women for decades and are mostly safe.
“This is a really big step forward in recognizing the autonomy of women to make decisions about their own health care,” said Dr. Emily Miller, an obstetrician at Northwestern University and a member of the Society for Maternal and Fetal Medicine Covid-19 Task Force.
With the first doses of the vaccine reserved for healthcare workers and residents of long-term care facilities, FDA approval will most directly affect the estimated 330,000 pregnant and breastfeeding healthcare workers in the United States.
“I am incredibly supportive of the FDA’s decision to keep the door open to Covid vaccination for pregnant and breastfeeding workers,” said Ruth Faden, a bioethicist at Johns Hopkins University in Baltimore.
Some healthcare workers are at high risk for Covid-19, either because they come into intensive contact with the virus as a result of their work – for example cleaning the rooms of sick patients – or because they live in low-income houses with several generations, Dr. Said thread.
“We need to be able to give women the opportunity to reconsider this with anyone who provides obstetric assistance,” she said.
Health organizations should also help their employees weigh the risks and accommodate women who are uncomfortable on the front lines, she added.
None of the clinical vaccine studies have included pregnant or breastfeeding women, or even women planning a pregnancy. Some trials are expected to begin in January.
Still, the American College of Obstetrics and Gynecology, the SMFM, and other organizations have urged the FDA to provide access to the vaccine for pregnant and breastfeeding people.
At a meeting Thursday to review Pfizer data for approval for emergency use, Dr. Doran Fink, FDA deputy director for vaccine development, said the agency was open to the idea.
“We really have no data to suggest any risks to pregnant women or the fetus, but neither do we have any data to justify a contraindication to use in pregnancy at this point,” said Dr. Finch. “Within the framework of the EEA, you can then make your own decision together with your healthcare provider.”
The EEA has not endorsed the vaccine for pregnant or breastfeeding women, except that Pfizer should collect long-term data on the performance of the vaccine in pregnant women.
Since the 1960s, pregnant women have been encouraged to receive vaccines against influenza and other diseases. These women are generally warned about live vaccines that contain weakened pathogens.
Even so, in some situations, the benefits of live vaccines outweigh the risks, said Dr. Denise Jamieson, an obstetrician at Emory University in Atlanta and a member of the ACOG Committee on Covid Vaccines.
“We have a long track record of vaccinating pregnant women and almost all vaccinations are very safe,” said Dr. Jamieson.
Dr. Jamieson said she was “disappointed that the FDA wasn’t more explicit,” but encouraged that “there is no explicit contraindication to pregnancy, which is good”.
Healthcare providers should be ready to advise pregnant patients in deciding whether to immunize them based on the patient’s potential exposures and underlying conditions such as diabetes and obesity, added Dr. Jamieson added.
“A woman who can stay at home with no other children and no one to work around the house is very different from an important worker who has to go out every day and be with other people,” she said.
The road to a coronavirus vaccine ›
Answers to your vaccine questions
As the coronavirus vaccine nears U.S. approval, here are some questions you may be wondering about:
-
- If I live in the US, when can I get the vaccine? While the exact order of vaccine recipients may vary from state to state, most doctors and residents of long-term care facilities will come first. If you want to understand how this decision is made, this article will help.
- When can I get back to normal life after the vaccination? Life will only get back to normal once society as a whole receives adequate protection against the coronavirus. Once countries have approved a vaccine, they can only vaccinate a few percent of their citizens in the first few months. The unvaccinated majority remain susceptible to infection. A growing number of coronavirus vaccines show robust protection against disease. However, it is also possible that people spread the virus without knowing they are infected because they have mild symptoms or no symptoms at all. Scientists don’t yet know whether the vaccines will also block the transmission of the coronavirus. Even vaccinated people have to wear masks for the time being, avoid the crowds indoors and so on. Once enough people are vaccinated, it becomes very difficult for the coronavirus to find people at risk to become infected. Depending on how quickly we as a society achieve this goal, life could approach a normal state in autumn 2021.
- Do I still have to wear a mask after the vaccination? Yeah, but not forever. The two vaccines that may be approved this month clearly protect people from contracting Covid-19. However, the clinical trials that produced these results were not designed to determine whether vaccinated people could still spread the coronavirus without developing symptoms. That remains a possibility. We know that people who are naturally infected with the coronavirus can spread it without experiencing a cough or other symptoms. Researchers will study this question intensively when the vaccines are introduced. In the meantime, self-vaccinated people need to think of themselves as potential spreaders.
- Will it hurt What are the side effects? The vaccine against Pfizer and BioNTech, like other typical vaccines, is delivered as a shot in the arm. The injection is no different from the ones you received before. Tens of thousands of people have already received the vaccines, and none of them have reported serious health problems. However, some of them have experienced short-lived symptoms, including pain and flu-like symptoms that usually last a day. It is possible that people will have to plan to take a day off or go to school after the second shot. While these experiences are not pleasant, they are a good sign: they are the result of your own immune system’s encounter with the vaccine and a strong response that ensures lasting immunity.
- Will mRNA vaccines change my genes? No. Moderna and Pfizer vaccines use a genetic molecule to boost the immune system. This molecule, known as mRNA, is eventually destroyed by the body. The mRNA is packaged in an oily bubble that can fuse with a cell, allowing the molecule to slide inside. The cell uses the mRNA to make proteins from the coronavirus that can stimulate the immune system. At any given moment, each of our cells can contain hundreds of thousands of mRNA molecules that they produce to make their own proteins. As soon as these proteins are made, our cells use special enzymes to break down the mRNA. The mRNA molecules that our cells make can only survive a few minutes. The mRNA in vaccines is engineered to withstand the cell’s enzymes a little longer, so the cells can make extra viral proteins and trigger a stronger immune response. However, the mRNA can hold for a few days at most before it is destroyed.
Women considering pregnancy should receive both doses of vaccine before trying to get pregnant, she added.
When first introduced, mostly pregnant health care workers must weigh the benefits and potential risks. By the time the vaccine is available to pregnant vital workers or women in the general population, experts say much more data should be available.
“The big question, which we don’t really know yet, is whether it actually crosses the placenta,” said Dr. Geeta Swamy, an obstetrician at Duke University in Durham, NC and a member of ACOG’s Covid Vaccine Group, regarding the vaccine. “To be honest, the most comforting thing would be to see some of the animal data.”
DART (developmental and reproductive toxicity) studies are carried out on animals to assess the possible effects of a vaccine on a fetus. This data is usually required for the licensing of a vaccine, but not for an EEA
Animal studies would ideally have been conducted as soon as safety data on the vaccines were available and before companies began large studies, said bioethicist Dr. Thread. However, at the FDA meeting Thursday, Pfizer officials indicated the animal data would be available by the end of the year.
(Moderna didn’t respond to questions about its animal testing schedule, and it was unclear whether AstraZeneca and Johnson & Johnson had started theirs.)
“The vaccines behind it – if you haven’t started your DART studies, you should start them yesterday,” said Dr. Thread.
The experts were particularly excited about the prospect that breastfeeding women could receive the vaccine. “The biological plausibility for the risk of harm to an infant from breastfeeding is extremely low,” said Dr. Swamy.
By the time an antigen – the essential part of the new vaccine – was injected into a woman’s arm to get through her bloodstream and into breast milk, the antigen would dissolve.
“There is no good reason to believe that vaccinating children is unsafe,” added Dr. Swamy added. “To be honest, we don’t have any pediatric studies trying to figure out the right dosage.”
Some women have been breastfeeding for years, and it can have devastating effects on babies, especially in low- and middle-income countries, experts say.
“I would appreciate the fact that the FDA has recognized that in the absence of data and relevance, bilateral decisions should be made between patients and their providers,” said Dr. Swamy. “We’re talking about women who are adult individuals, right?”